
Quality Improvement Initiatives
Implement systematic, evidence-based improvements to enhance clinical outcomes
Clinical Quality Improvement Studies (Direct and Private Sector Care)
Clinical quality improvement (QI) studies systematically improve patient care, safety, and outcomes by implementing evidence-based practices and reducing process variation. These studies often use iterative, fast-paced methods like the Plan-Do-Study-Act (PDSA) cycle, rather than long-term, controlled research designs. Examples include reducing infections, shortening hospital stays, and enhancing care coordination.
PROTeam Management provides a range of quality improvement studies to assess patient care for the purpose of improvement through peer analysis, intervention, resolution of the problem, and follow-up.
Studies often target the six dimensions of healthcare quality (STEEEP): Safety, Timeliness, Efficiency, Effectiveness, Equity, and Patient-centeredness.
Examples of Quality Improvement Initiatives:
- Reducing Harm: Initiatives aimed at decreasing surgical site infections, catheter-associated urinary tract infections, or medication errors.
- Efficiency Improvements: Shortening patient wait times, reducing hospital lengths of stay, and improving discharge processes.
- Documentation & Coordination: Enhancing electronic medical record (EMR) documentation and improving care transitions between departments
Starting a quality improvement (QI) initiative involves defining a clear, measurable aim, forming a multidisciplinary team, and using data to identify problems. Utilize the “Model for Improvement” by setting goals, choosing measures, and testing changes via small-scale PDSA (Plan-Do-Study-Act) cycles to ensure success
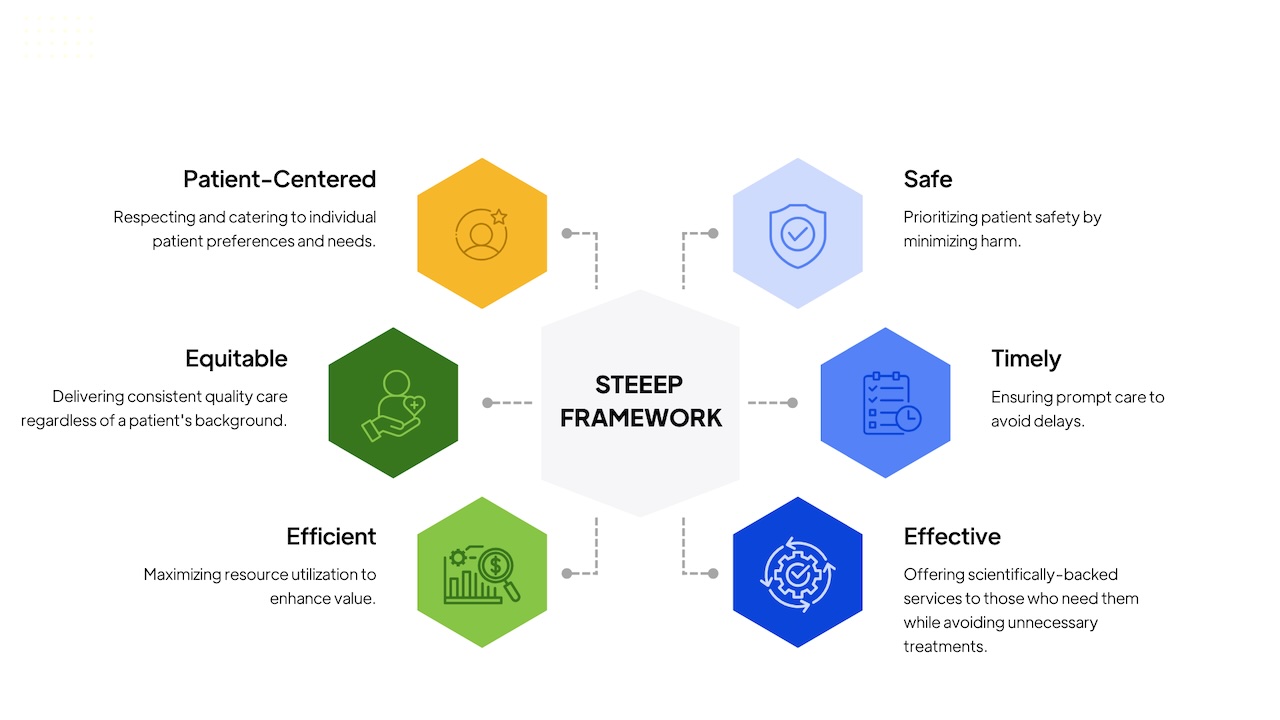
STEEEP Model
STEEEP is an Institute of Medicine (IOM) framework for high-quality healthcare, focusing on six core aims: Safe, Timely, Effective, Efficient, Equitable, and Patient-centered care. It aims to reduce medical errors, improve patient experiences, and optimize care delivery by aligning clinical practices with patient needs and evidence-based medicine, often supported by technology.